Meet The Team

Dr. Sanford Altman
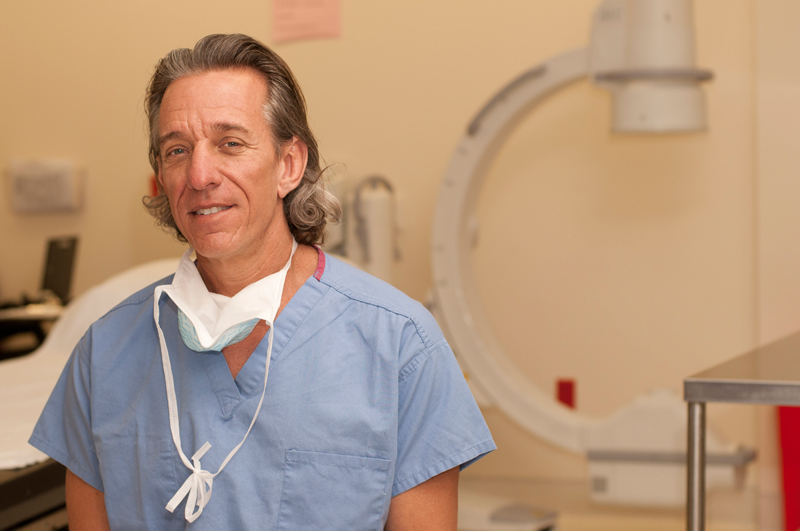
Sanford D. Altman, M.D. is the founder and Medical Director of Open Access. As a pioneer interventionalist and expert on dialysis access, he has been performing dialysis access procedures since 1994 and has successfully performed over 40,000 procedures on dialysis patients. Dr. Altman has published and lectured in the area of dialysis access care and management. He is actively involved in dialysis access research as well as the development of new products for dialysis patients. Dr. Altman strives to provide the best quality care to his patients, something he has done in the tri-county area for over two decades. He serves on many national committees pertaining to dialysis access care and is a lifetime member of the American Association of Kidney Patients (AAKP).
Publications | Professional Affiliations | Presentations (Lecture Circuit) |Media Spokesperson Contact
Publications
Stent Graft Versus Balloon Angioplasty for Failing Dialysis Access Grafts
Authors: Haskal ZJ, Trerotola S, Dolmatch B, Schuman E, Altman S, Mietling S, Berman S, McLennan G, Trimmer C, Ross J, Vesely T.
N Engl J Med. 2010 Feb 11;362(6):494-503. doi: 10.1056/NEJMoa0902045.
Authors: Altman SD, Ross JJ, Work J.
J Vasc Access. 2008 Oct-Dec;9(4):236-40.
Summary: Catheter-related blood stream infections pose a significant risk for patients living with vascular catheters. The cost to manage these infections is substantial. Although the etiology of these infections is multifactorial, tap water has been implicated as a significant causative factor. This retrospective review evaluates the effectiveness of a surgical dressing, the CD-1000, at protecting catheters and exit site wounds from fluid and debris when patients engage in high risk activities like showering.
Interventional Care of the Hemodialysis Patient: It’s About Quality
Authors: Trerotola SO, Gray R, Brunner M, Altman S.
J Vasc Interv Radiol. 2001 Nov;12(11):1253-5.
Accuracy and Reproducibility of Urea Recirculation in Detecting Haemodialysis Access Stenosis
Authors: Paulson WD, Gadallah MF, Bieber BJ, Altman SD, Birk CG, Work J.
Nephrol Dial Transplant. 1998 Jan;13(1):118-24.
Summary: There is wide disagreement among studies that have evaluated the accuracy of urea recirculation (UR) in detecting vascular access stenosis. The 3-site method (UR3) has been discredited and replaced by the 2-site method (UR2), but few studies have evaluated UR2. METHODS: We compared the accuracies of UR2 and UR3 in detecting stenosis in 59 haemodialysis patients during a 12-month period. All patients were studied without regard to clinical suspicion of stenosis. Stenosis (> or = 50% luminal narrowing) was diagnosed by duplex ultrasound and confirmed by angiography. The reproducibility of UR2 was determined by computing its total standard deviation (SDTOT) from measurements during three dialysis sessions over a 15-day period. RESULTS: Stenosis was found in 32% of 124 access studies (mean luminal narrowing = 58%, range = 50%-83%). The mean UR values of stenotic accesses were only slightly higher than non-stenotic accesses for both UR2 (5.6% vs 2.9%, P < 0.01) and UR3 (13.1% vs 11.2%, P = 0.22). An increase in blood pump speed from 300 to 425 ml/min did not improve detection of stenosis by UR2. There were no UR thresholds that could adequately separate the presence of stenosis from its absence. The SDTOT of UR2 was 3.8%, indicating that a patient’s UR2 measurement may vary over a range of 16% (+/- 2SDTOT = +/- 8%). CONCLUSION: Stenosis of the haemodialysis access does not predictably cause recirculation, and the reproducibility of the UR2 measurement is poor.
A Practical Approach for Diagnosis and Treatment of Central Venous Stenosis and Occlusion
Author: Altman SD.
Semin Vasc Surg. 2007 Sep;20(3):189-94. Review.
Summary: Treating symptomatic central venous stenosis and occlusion is a challenge for those caring for patients with end stage renal disease. With the increase incidence and decrease mortality of end stage renal disease, there are more patients presenting for vascular access procedures. Although there has been a significant increase in the prevalence of fistulae in the United States over the last several years, many of these patients require central venous catheters during the fistula maturation process. The use of these catheters, along with the increase in the diameters of many of these catheters over the last several years, has likely played a significant role in the development of symptomatic central venous stenosis and occlusion. In this article the origin or central venous stenosis and occlusion will be reviewed along with a practical approach on how to best manage this disease process.
Portal Vein Thrombolysis and Closure of Competitive Shunts Following Liver Transplantation
Authors: Durham JD, LaBerge JM, Altman S, Kam I, Everson GT, Gordon RL, Kumpe DA.
J Vasc Interv Radiol. 1994 Jul-Aug;5(4):611-5; discussion 616-8.
Professional Affiliations
- American Association of Kidney Patients (AAKP)
- American College of Phlebology (ACP)
- American College of Radiology (ACR)
- American Institute of Ultrasound in Medicine (AIUM)
- American Medical Association (AMA)
- American Roentgen Ray Society (ARRS)
- American Society of Diagnostic and Interventional Nephrology (ASDIN)
- American Society of Nephrology (ASN)
- Florida Radiological Society (FRS)
- International Society of Nephrology (ISN)
- National Kidney Foundation (NKF)
- Radiological Society of North America (RSNA)
- Society of Interventional Radiology (SIR)
- Vascular Access Society of the Americas (VASA), founding board member
Presentations (Lecture Circuit)
1994 | 1995 | 1996 | 1997 | 1998 | 1999
2000 | 2001 | 2002 | 2003 | 2004 | 2005 | 2006 | 2007 | 2008 | 2009 | 2010 | 2011 | 2012 | 2013 | 2014
1994
Ohio State University
Vascular Access for Hemodialysis: Ultrasound-Guided Angioplasty of Hemodialysis Access Stenosis
Arizona Nephrology Society
Percutaneous Management of Failing Hemodialysis Access
Florida Renal Coalition Patient Service Program
Vascular Access Latest Options
1995
LSU Hemodialysis Access Management Seminar
Maintenance Angioplasty of Hemodialysis Access Stenosis
Florida Renal Nurses Association
Maintenance Angioplasty of Hemodialysis Access Stenosis
Florida Society of Nephrology
Maintenance Angioplasty of Hemodialysis Access Stenosis
1996
Ohio State University-Vascular Access for Hemodialysis
Maintenance Angioplasty for Hemodialysis Access Stenosis in the Mobile Setting
Vivra Renal Care-Medical Directors meeting
Hemodialysis Access Ultrasound Surveillance Combined with Maintenance Angioplasty
Benefits of a Maintenance Program
American Society of Nephrology
Maintenance Angioplasty of Hemodialysis Access Stenosis in the Mobile Setting
1997
American Society of Nephrology
Access Surveillance, Duplex Doppler Imaging and Early Percutaneous Intervention: Improved Access Patency and Adequacy of Dialysis
Total Renal Care Regional Directors Meeting
Vascular Access for Hemodialysis: Placement and Maintenance
Renal Management Strategies Medical Advisory Board
Access Surveillance, Duplex Doppler Imaging and Early Percutaneous Intervention: Improved Access Patency and Adequacy of Dialysis
1998
Total Renal Care
Advances in Dialysis Care: The Future of Hemodialysis Access Management
ASAIO
Duplex Doppler Imaging and Early Percutaneous Intervention: Improved Access Patency and Adequacy of Dialysis
Northeastern Conference on Vascular Access for Hemodialysis
Elective Angioplasty of Hemodialysis Access Stenosis in a Mobile Setting
1999
Puerto Rico Nephrology Society
Vascular Access for Hemodialysis, Fact or Fiction
National Kidney Foundation
Monitoring of Vascular Access: Comparison of Different Techniques
American Society of Nephrology
Monitoring of Vascular Access: Comparison of Different Techniques
Prospective Comparison of Access Flow Measurements Using Conventional Color Duplex Doppler Ultrasound and Ultrasound Dilution Techniques
2000
SCVIR
Alternative Practice Model: How I’ve Done It
2001
SCVIR
Freestanding Outpatient Center: Should You Have Your Own?
2003
SIR
Lessons Learned: Complex Venous Access
ESRD Network of Florida Annual Meeting
Dialysis Access Placement and Maintenance: KDOQI and Beyond
AIM Symposium
Percutaneous Declotting of Native Fistulae: Experience with the Xpeedior Catheter
Hands-On Workshop: Thrombectomy Devices, New Tools for Dialysis Graft Declotting
2004
SIR
Outpatient IR: Time to Roll
How to Set up a Lab: Soup to Nuts
IR Traditional Model vs. Alternative Models
My Experience/My Center
2006
SIR
Workshop: Hemodialysis Access Overview
2007
SIR
Workshop: Hemodialysis Access Techniques
Alternative Practice Models
VASA
Declotting of Grafts and Fistulae
ASDIN
Cephalic Arch Stenoses
SFSS
Freestanding Access Center Development
Vascular Access Difficult Cases
AIM/Veith
Ultrasound Imaging In Vascular Access
Prevention of Catheter -Related Infections
2008
SIR
Workshop: Hemodialysis Access Techniques
2009
VASA
Catheter Workshop
Ultrasound Workshop
Cephalic Arch Stenosis
Endovascular Treatment of Complications
Lifeline Vascular Access Physician Operators Forum
Ultrasound of Dialysis Access
Complex Access Intervention
2010
SIR
Dialysis Access Interventions
2011
AIM/Veith
Fistula Declotting and Intervention
2012
CIDA
Fistula Declotting Techniques, Complex Vascular Access
Media Spokesperson Contact
Lisa Gdowski
Marketing Manager
Lifeline Vascular Access
Phone: 847-388-2098
